
Dr Colum Nolan
Senior Consultant Spine & Neurosurgeon
MB, BCh, BAO, LRCPSI, MRCSI, FRCSI (Neurosurgery)
Persistent spine-related pain can affect daily activities, work, and overall quality of life. For some individuals, pain may continue despite medication, physiotherapy, or injection-based treatments. In selected cases, radiofrequency ablation may be considered as part of a structured, non-surgical pain management approach.
This page explains what radiofrequency ablation involves, how it is performed, and how it fits into a broader spine care plan.
Chronic spine pain may arise from irritation of specific nerves that transmit pain signals from joints or structures within the spine. This type of pain is often:
When pain is traced to specific nerves rather than widespread inflammation, targeted pain management options may be discussed.
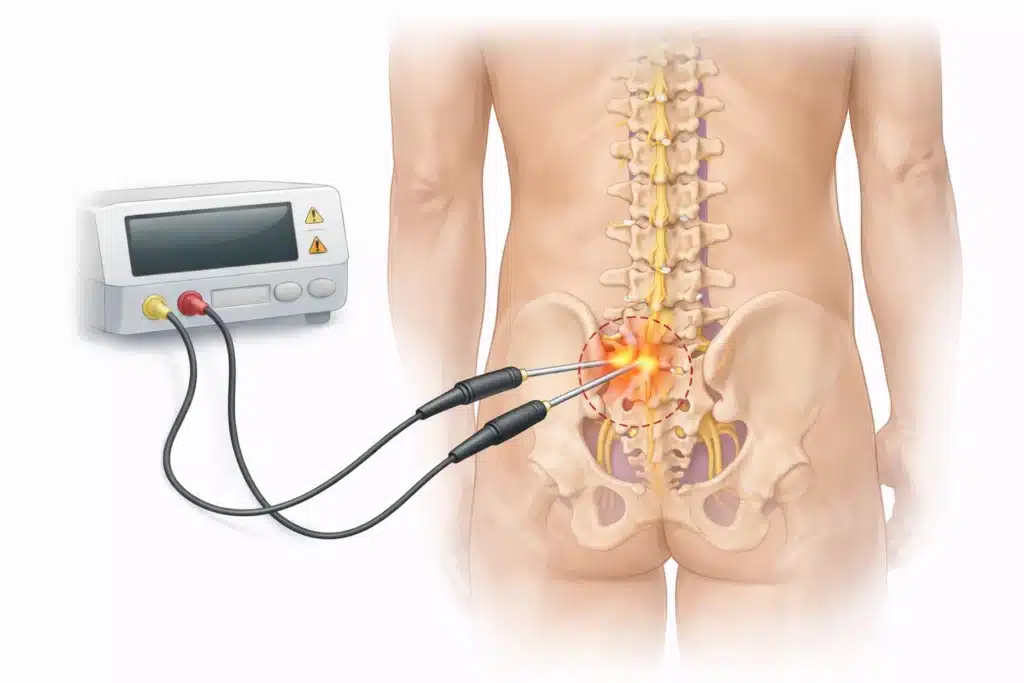
Radiofrequency ablation, often referred to as RFA, is a non-surgical, needle-based procedure used to reduce pain by interrupting pain signals from selected spinal nerves.
It does not involve inserting any implant, device, or module into the body. Instead, controlled radiofrequency energy is delivered through a specialised needle placed close to the targeted nerve. This reduces the nerve’s ability to transmit pain signals to the brain.
Radiofrequency ablation does not alter the structure of the spine and is used solely for pain management.
Radiofrequency ablation is usually carried out as a day procedure.
In general:
The procedure typically takes a short time, followed by a brief observation period before going home.
Radiofrequency ablation is usually considered after diagnostic nerve blocks have been performed. These blocks help confirm whether a specific nerve is responsible for the pain.
If temporary pain relief is achieved after a nerve block, it suggests that the same nerve may respond to longer lasting pain interruption with radiofrequency ablation. This stepwise approach helps ensure appropriate patient selection.
Radiofrequency ablation reduces the nerve’s ability to transmit pain signals, but nerves can recover over time. This means that pain relief is not permanent, and symptoms may return months later in some individuals.
If pain returns, further assessment is required before considering additional treatment.
Radiofrequency ablation may be used in the management of selected spine-related pain conditions, including:
It is not suitable for all types of spine pain and is recommended only when clinical findings support its use.
When performed by trained specialists, radiofrequency ablation is generally considered safe. As with any medical procedure, potential risks exist, though serious complications are uncommon.
Possible risks include:
Your doctor will review individual suitability and risks before proceeding.
At Oxford Spine and Neurosurgery Centre, radiofrequency ablation is used selectively as part of an individualised pain management plan. Decisions are guided by careful clinical assessment, symptom patterns, and response to prior treatments.
Care is led by Dr Colum Nolan, Senior Consultant Neurosurgeon, with emphasis on appropriate patient selection, clear explanation, and thoughtful sequencing of care options.
Radiofrequency ablation is a non-surgical, needle-based procedure used to help manage selected types of spine-related pain. It does not involve implants or permanent devices and does not alter the structure of the spine. When used appropriately, it may reduce pain signals, improve comfort, and support daily function as part of a broader pain management plan.
Medical Disclaimer
This page is intended for general educational purposes only and does not constitute medical advice. Information provided is not a substitute for professional medical consultation, diagnosis, or treatment. Suitability for radiofrequency ablation or any spine-related procedure must be determined by a qualified medical practitioner following appropriate clinical assessment.
Dr Colum Nolan is a Senior Consultant Neurosurgeon with over 20 years of experience, specialising in minimally invasive spine (keyhole) surgery and other spine procedures.
A graduate of the Royal College of Surgeons in Ireland, Dr Nolan underwent neurosurgical training in Ireland and Australia, followed by a fellowship in complex spine surgery at Addenbrooke’s Hospital, Cambridge, as well as rotations at the Orthopaedic Spine Unit in Norfolk and Norwich Hospital.
Dr Colum is committed to delivering compassionate, patient-centred care, combining surgical precision with a genuine dedication to improving his patients’ quality of life.

Make an Enquiry or Request an Appointment
Our friendly team is here to serve you. For urgent enquiries and appointment requests, please call or WhatsApp us directly.