
Dr Colum Nolan
Senior Consultant Spine & Neurosurgeon
MB, BCh, BAO, LRCPSI, MRCSI, FRCSI (Neurosurgery)
You bend forward to pick something up and feel a sudden jolt of pain shoot from your lower back into your buttock and down your leg. Sitting through a meeting becomes uncomfortable because the ache spreads into your calf. At night, your foot tingles, and you wonder why the discomfort seems to follow the same line each time.
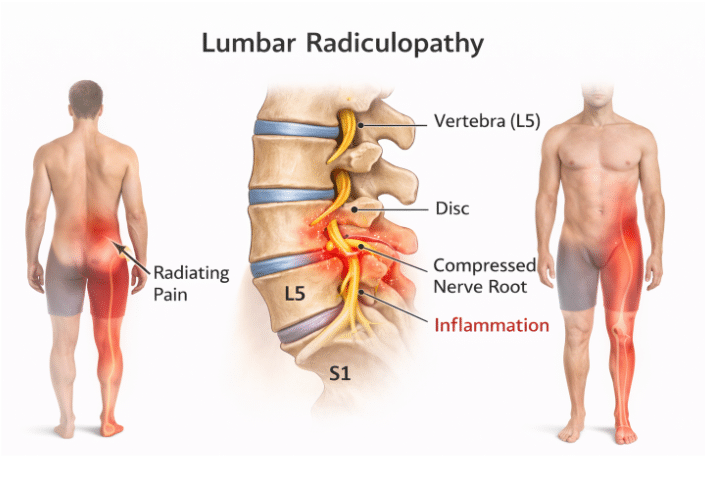
Pain that travels below the lower back and into the leg is often different from a simple muscle strain. When a spinal nerve in the lumbar region becomes irritated or compressed, it can trigger sharp, burning or electric-like sensations, along with numbness or weakness. This pattern is known as lumbar radiculopathy, commonly described as a pinched nerve in the back. Understanding why the pain radiates, and what may be causing the pressure on the nerve, is an important first step towards appropriate assessment and management.
Lumbar radiculopathy occurs when a nerve root in the lumbar spine becomes compressed or inflamed. These nerve roots carry signals that control muscle movement in the legs and transmit sensation from the skin of the lower limbs.
When a nerve root is irritated, pain and altered sensation can be felt along the pathway of that nerve, commonly from the lower back into the buttock, thigh, calf, and sometimes the foot. Tingling and numbness are frequent, and muscle weakness may develop if compression is significant or prolonged.

A range of conditions can place pressure on a nerve root in the lower back. Some are related to age-related changes in the spine, while others are less common. Understanding the underlying cause helps guide appropriate assessment and treatment.
One of the most common causes is a herniated (slipped) disc. A spinal disc has a softer centre and a tougher outer layer. If the disc bulges or a fragment protrudes, it can press on a nearby nerve root and trigger inflammation. This is often associated with leg pain that may be worse than the back pain.
Lumbar radiculopathy can develop suddenly or gradually, and symptoms may fluctuate.
Altered sensation is common, including tingling (“pins and needles”), burning, or numbness in a pattern that often follows the pain distribution. These sensations may occur with pain or on their own.
Muscle weakness can develop if nerve signalling is more significantly affected. Examples include difficulty lifting the foot, weakness when climbing stairs, or reduced ability to stand on tiptoes.
Seek urgent assessment if any of the following appear or worsen:
Not all leg pain comes from a pinched nerve. However, lumbar radiculopathy is more likely when pain:
Other conditions (such as hip problems, peripheral nerve entrapment, vascular issues, or muscular strain) can mimic similar symptoms, which is why proper assessment matters.
Lumbar radiculopathy can affect anyone, but certain factors increase risk.
Degenerative changes in discs and joints become more common with age, increasing the likelihood of narrowing around nerves. Disc herniation can also occur in younger adults, especially after strain or injury.
Factors that may increase risk include:
A history of radicular pain can increase the chance of recurrence, particularly if underlying degenerative changes persist.
Lumbar radiculopathy is diagnosed through a combination of clinical assessment and, when necessary, imaging or specialised tests. In many cases, a clear diagnosis can be made based on your symptoms and physical examination alone. Additional investigations are usually reserved for persistent, severe, or unclear cases.
You may be asked to describe:
Some cases improve with time and conservative care. When treatment is needed, it usually starts with non-surgical options.
Lumbar radiculopathy can significantly affect comfort, mobility and daily function. Radiating leg pain, numbness or weakness may interfere with work, sleep and routine activities. Because other spinal and non-spinal conditions can cause similar symptoms, a detailed clinical assessment is essential to determine the severity of nerve involvement and identify the underlying cause, guiding appropriate treatment.
At Oxford Spine & Neurosurgery Centre, Dr Colum Nolan and the specialist team provide comprehensive, evidence-based care tailored to each individual. Management plans are developed with attention to symptom severity, functional goals and long-term spinal health, whether that involves structured non-surgical treatment or, in selected cases, surgical intervention. If you are experiencing persistent leg pain, tingling or weakness, arrange a consultation with Dr Nolan for personalised guidance and a clear plan for your next steps towards recovery.
Dr Colum Nolan is a Senior Consultant Neurosurgeon with over 20 years of experience, specialising in minimally invasive spine (keyhole) surgery and other spine procedures.
A graduate of the Royal College of Surgeons in Ireland, Dr Nolan underwent neurosurgical training in Ireland and Australia, followed by a fellowship in complex spine surgery at Addenbrooke’s Hospital, Cambridge, as well as rotations at the Orthopaedic Spine Unit in Norfolk and Norwich Hospital.
Dr Colum is committed to delivering compassionate, patient-centred care, combining surgical precision with a genuine dedication to improving his patients’ quality of life.

Make an Enquiry or Request an Appointment
Our friendly team is here to serve you. For urgent enquiries and appointment requests, please call or WhatsApp us directly.