
Dr Colum Nolan
Senior Consultant Spine & Neurosurgeon
MB, BCh, BAO, LRCPSI, MRCSI, FRCSI (Neurosurgery)
A “slipped vertebra” usually refers to spondylolisthesis, where one vertebra slips forward over the one below it. This shift can narrow the space where spinal nerves exit, leading to nerve irritation or compression and pain that may travel into the buttock or leg.
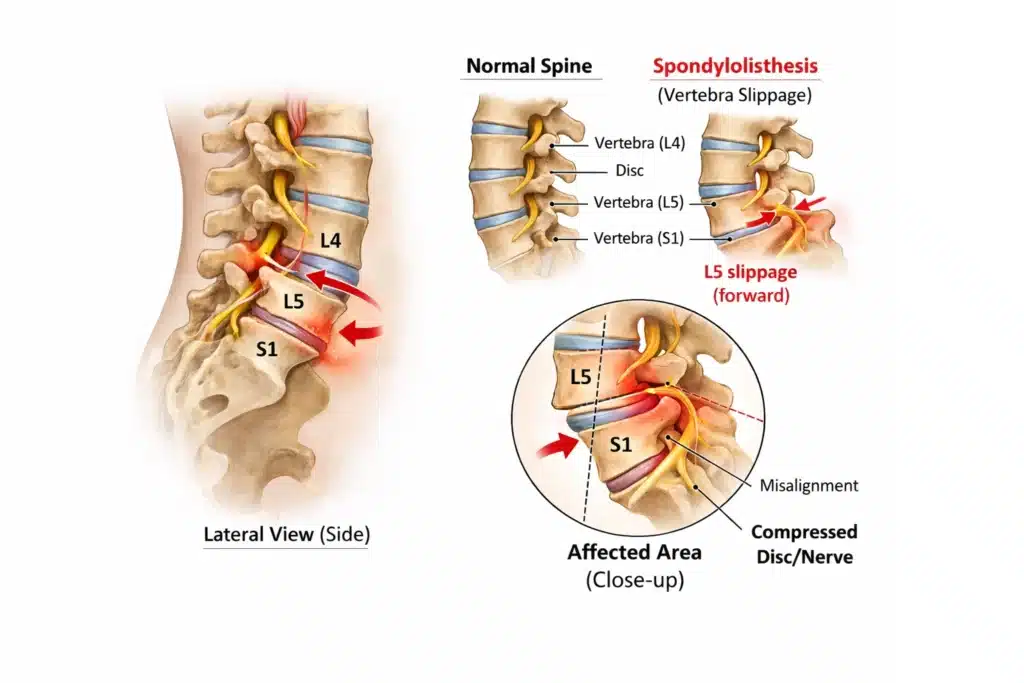
Spondylolisthesis most commonly occurs in the lumbar spine (lower back). Some people have a slip found on X-ray but feel fine. Others develop symptoms because the slip:
The impact depends on factors such as the degree of slip, whether there is instability, and whether the slip contributes to spinal canal or foraminal narrowing.
Spondylolisthesis can narrow the space where nerves exit, and symptoms may travel along the nerve pathway.
Common features include:
Some people also notice reduced walking tolerance, or symptoms that fluctuate with posture and activity.

A detailed history and examination looking at:

Treatment is typically stepwise, guided by your symptoms, function, and whether nerves are involved.
Surgery is usually considered when:
The goals of surgery are to relieve pressure on nerves (decompression) and, when needed, stabilise the spine (fusion).
This page is for general education and does not replace a medical consultation. If you have severe symptoms, worsening weakness, or bladder/bowel changes, seek urgent medical attention.
Dr Colum Nolan is a Senior Consultant Neurosurgeon with over 20 years of experience, specialising in minimally invasive spine (keyhole) surgery and other spine procedures.
A graduate of the Royal College of Surgeons in Ireland, Dr Nolan underwent neurosurgical training in Ireland and Australia, followed by a fellowship in complex spine surgery at Addenbrooke’s Hospital, Cambridge, as well as rotations at the Orthopaedic Spine Unit in Norfolk and Norwich Hospital.
Dr Colum is committed to delivering compassionate, patient-centred care, combining surgical precision with a genuine dedication to improving his patients’ quality of life.

Make an Enquiry or Request an Appointment
Our friendly team is here to serve you. For urgent enquiries and appointment requests, please call or WhatsApp us directly.